|
By Colette Corr We know that motion is lotion, but how do we best support our lower back when feeling pain there? This pain could be caused by injury to a muscle (strain) or ligament (sprain), for example from improper lifting, poor posture, or lack of regular exercise. Other causes that might require more support include radiculopathy (a pinched nerve), arthritis or disc injury. While it’s important to get a diagnosis for certain conditions, remember that many types of lower back pain go away on its own in two to four weeks. Here are some stretches to help increase blood flow to the area, and soothe tight muscles and connective tissue. Yoga has also been associated with improved body awareness and resilience, including pain acceptance and coping. The yoga you do for your lower back will depend on whether the pain you experience there is triggered by flexion (folding forward) or extension (bending back). If folding forward triggers the pain, then focus on extension (Sphinx, Locust). Or if bending back is the issue, then focus on flexion (Child’s Pose). The first two exercises, Mountain and Cat/Cow, can be done by anyone. 1. Extend the spine in Mountain (Tadasana) This is good for any back, as back pain can frequently be associated with certain structures in the spine being too close to each other. Stand with your feet stacked underneath your hips, your arms by your sides a little way away from the body and palms facing the front, or choose to press your palms together at the chest. Have a little softness at the knees, draw your shoulder blades back and down, open up the chest, and visualise your spine lengthening. You can also practice this pose while sitting, if standing is not comfortable for you. Benefits: this pose improves balance, posture and awareness of your body in space (proprioception). It also increases space between each vertebrae through vertebral extension, mobilises your spine, and stimulates the nervous system. 2. Mobilise the spine with Cat/Cow Start in a kneeling position (also known as Table Top) and stack wrists under shoulders and knees under hips. With the inhale, tilt your pelvis away from the ground, and open up your chest and neck (Cow). With the exhale, tuck your pelvis in, arch your back, and bring your chin closer to your chest (Cat). Repeat 10 times. There’s no need to go to the end of your range of motion: just undulate your spine and with the breath and enjoy the feeling of movement. You can also practice this pose while sitting. Benefits: this gentle, accessible backbend stretches and mobilises your spine and spinal muscles. It also stretches your torso, shoulders, and neck. Caution: If either Cat or Cow aggravate your lower back, you can practice Table Top to Cat, or Cow to Table Top instead. 3. Extend the spine in Sphinx pose Lie on your belly, legs side by side, tailbone gently tucked, and glutes firm but not clenched. Stack your elbows under your shoulders and your forearms on the floor parallel to each other. Inhale and lift your upper torso and head away from the floor into a mild backbend. Take a few breaths here, then, then slowly lower your torso and head to the floor. Benefits: strengthens the spine, promotes natural curvature of the lower back (which can be flattened by prolonged sitting), and stretches chest, lungs, shoulders, and abdomen. Caution: Listen to your body. If you start to feel pain coming into the pose, this is where you stop. You can pause at the threshold before the pain begins, or you can discontinue the pose. Avoid if you have facet joint injury. 4. Strengthen the core with Half Locust If Sphinx is comfortable for you, you can take it further with Half Locust. Start on your belly, legs parallel and ideally together, and reach your hands back, palms down. Broaden your collarbone and draw the shoulder blades back and down. Inhale and engage your abs, which will lift your belly lift towards your spine. Then, activate your inner thighs. With the exhale, gently squeeze your glutes to lift your legs off the ground and keep them there as you breath. Take 3 long, slow breaths, and lower on the last exhale. If comfortable in Half Locust, you can come to full Locust but lifting the upper body up into a Sphinx-like shape, but keeping your palms by your side. Only do this if you can keep the glutes and core engaged at the same time. Benefits: works glutes and abdominals, tones thoracic spine. Caution: as for Sphinx. 5. Flex the spine with Child’s Pose From Table Top, on the exhale, draw the buttocks back towards the heels. For additional comfort, you can do so over a lengthened bolster. Benefits: This pose improves spinal flexibility, relieves stress and improves circulation to the back. These yoga poses are generally safe for most people to enjoy for stretching out the lower back. As with any new exercise, if you are already having significant pain, please book a time to see one of our team for assessment and treatment, and we can advise you on the most appropriate exercises for your current condition, and guide you through any safe modifications to these exercises.
By Duke Autret Many, if not most people will have heard of, or may even have experienced sciatic pain or sciatica, but what is it exactly? Let’s explore. Sciatica is a term that gets thrown around alot but the fact is that it’s quite a vague term which is used simply to describe any condition where the symptoms involve pain running from the lower back down either one or both legs (potentially all the way down to the foot). Pain types can be sharp, shocking, tingly, numb, cause pins and needles, or cause pinching or catching sensations on movements.  So in fact Sciatica describes not one single condition, but rather a set of symptoms, and that these symptoms that we call Sciatica can be the result of a number of different mechanisms or conditions. To be more precise, Sciatic refers to the name of the nerves which branch out from origins in the lower spine/back and then splits into two Sciatic nerves - one for each leg, and thus innervates the muscles and structures of the legs. However this nerve can become vulnerable to irritation by pressure bearing on it from other structures, when this happens the experience is Sciatica! As mentioned before there can be a variety of reasons for this impingement on the Sciatic nerves and some examples can include pressure from a tight Piriformis muscle (which the sciatic nerve passes directly through or beneath), pressure from an Intervertebral Disc bulge/herniation of the lumbar spine (lower back), Stenosis which is the narrowing of the spinal canal, Spondylolisthesis which is the slipping of one vertebrae over the next and that can pinch the sciatic nerve, or Spondylosis, an arthritic joint degeneration at the lumbar vertebrae which may cause inflammation and subsequent pressure and irritation from that. As we can see, there are many ways in which the sciatic nerve can become impacted and the end result is the same experience and symptoms we call ‘Sciatica’. Some of these situations sound scary, but the majority of the time it is easy to get the pain under control while working with an experienced Myotherapist who can help guide you or refer you on if your condition is particularly acute or severe. Since the irritation that occurs to the Sciatic nerve is to do with some or other kind of pressure, then the priority for treatment becomes to create more space for the nerve to be free, as nerves also need to be able to slide and move with the rest of the body. Importantly, the treatment we use will be dependent on which of the various mechanisms are at play, but commonly any technique employed will be with the aim of creating more space for that nerve, and most often will involves treating the muscles of the lower back, pelvis, hips, glutes and back of the thighs and maybe even calves. Some of these techniques can include hands on options like remedial massage and myofascial release, or helpful nerve gliding movements that can help reduce the sensitivity of those nerves. And in situations where the symptoms are very acute, fresh and severe often Myofascial Dry Needling is a go-to in order to take the edge off and tone everything right down without adding any more undue pressure to the nerve/system. Myotherapists can also provide joint mobilisations to aid in better mobility of the lower back and hips. Mobilisations vary from manipulations - we won't be "cracking your bones", but gently encouraging rhythmic movement to return to your joints without any high velocity cracks or crunches. From here we would look at tailored exercises for your situation which could simply be stretches for a few key tight muscles to a full program to help build stability around the spine and support the structure for healthy nerve function. Some common exercises you might try could be deep abdominal work, diaphragm ‘weight-lifting’, the sphinx, Piriformis stretches, and Glute and Adductor strengthening. Our practitioners will demonstrate these types of exercises and how to safely do them while you're experiencing sciatica, and we can assist you in progressing them as preventative care exercises once the intensity of your pain has eased. If you or anyone you know is currently suffering with Sciatic pain, please come and see us, we are here to help. Just call or leave a message with us at the Simple Wellness Myotherapy clinic here in Rowville, or alternatively you can see our booking schedule and make an appointment yourself for a time that best suits.
Whats Causing This Pain Where My Lower Back And Hips Meet? It Could Be The Sacroiliac Joint10/8/2022
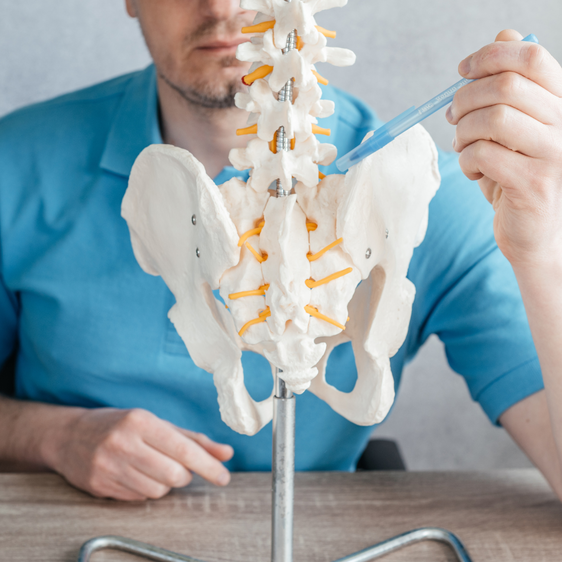
By Duke Autret Pain across the very base of your spine where your hips and lower back meet is very common. You can often pinpoint the pain as starting from "those two dimples at the lower back" and spreading out across the sides of the hips. Those two dimples, which aren't always visible on everyone, are where the back and hip join - specifically where the sacrum bone joins the iliac crest of the pelvis. This joint is called the Sacroiliac Joint. Sacroiliac Joint (SIJ) Dysfunction is an often used term to describe any issue that arises from some kind of problem at this joint, usually leading to the joint becoming inflamed, and which can commonly have subsequent implications such as sciatic pain (pain running down the leg) and/or pain from muscle spasms usually at the lower back and/or around the hip/s.
One reason for this is that the inflammation at the site of the Sacroiliac Joint may irritate the sciatic nerve much in the same way as a spinal disc problem can, although rather than perhaps a bulging intervertebral disc impinging on the sciatic nerve, instead it can be the chemical irritation and/or the pressure and compression caused by the swelling and inflammation of locals tissues and fluids. Then due to pain and irritation from the inflammation, a pain cycle may set in, with muscles spasming and tightening up in response. Our bodies are pretty marvellous in the way they try to protect us from a perceived problem, and that protection usually comes in the way of tensing, tightening or spasming. Consider if you were going to be punched in the gut, the first thing your body will naturally do before you probably even think about it is to tense your abdominals, draw in the arms and shoulders, and crunch forward in a protected position to lessen the blow. The SIJ does a similar process to try to protect around the joint area, which can lead to that persisting pain. Typically, an SIJ issue will present on just one side at a time, although it can be possible for the symptomatic side to swap from one side to the other, as when one SIJ is dysfunctional then the adjacent SIJ compensates and is therefore implicated. The good news is that you can get treatment for Sacroiliac Joint Dysfunction! Treatments we can provide to help when someone comes to us in an acute phase will revolve around ways of decreasing the muscle spasm and pain to the hip, pelvis and spinal regions, and to also advise you on the best ways to manage the joint inflammation itself and ‘deload’ the structures involved. The initial stages of the treatment are likely to involve some soft tissue work like remedial massage, myofascial release, cupping or dry needling, and can also involve taping the SIJ to support that area and give those really hard working muscles a chance for a break without leaving that joint feeling vulnerable. Then once these initial symptoms are under control we will guide you towards how to regain and develop the stability, mobility and control to the specific areas needed, which are likely to include the thigh muscles and the deep muscles of the trunk, abdominals, and back. Outside of any hands on treatments the lasting success of reversing this type of condition will depend also on the empowerment of you. We will advise you on the best rehab routine and provide a layered program over time so that you can progress at the right pace and without worrying about being overloaded with homework. Or alternatively, we can refer you to connect with local practitioners or instructors in clinical exercise or other modalities like yoga for example if you prefer or if help with motivation and supervision is what you need. Personally I enjoy working with SIJ pain since I used to suffer from a lot of it myself (and know how difficult it can be) and because I’ve learned how to best deal with it, to the point where I no longer suffer from this anymore. This has been a worthy investment for me and also a gift. I hope to share this with those who need it too. If you’d like to start down the road of finding ways to improve your own challenges with an SIJ issue, I am here to help. Just call or leave a message with us at the Simple Wellness Myotherapy clinic here in Rowville, our number is 03 8204 0970, or alternatively you can visit our website to see our booking schedule and make an appointment for yourself at a time that best suits you. Dry Needling is a manual therapy technique used by Myotherapists to help reduce pain and tension in muscles. We've previously discussed the similarities and differences between Dry Needling and Acupuncture, but you may still be wondering - how does Dry Needling actually work? The "Dry" Needle
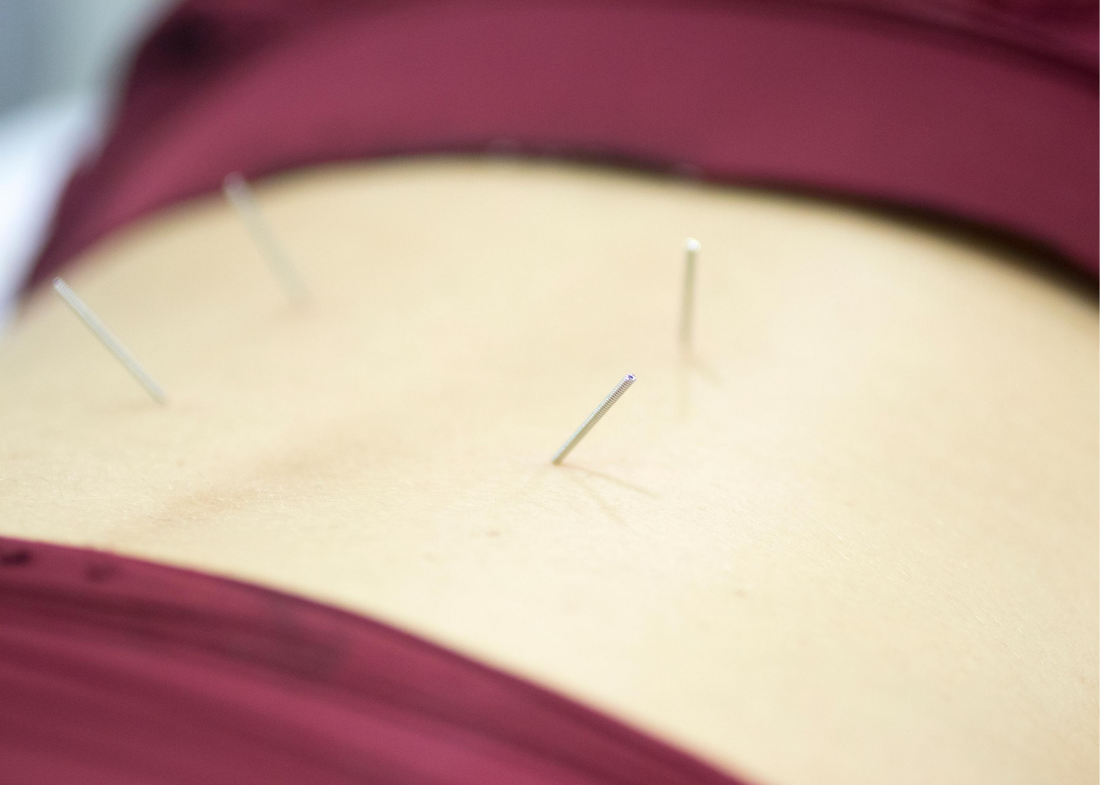
The reason they are called "dry" needles is to differentiate them from hollow needles like the ones used for blood tests or vaccinations. A dry needle can't inject or withdraw fluids from your body. The needles themselves are ultra thin and flexible. They come with a guide tube to allow us to place them with care and precision. All needles used for dry needling are single use only. Where We Apply It Myotherapists use dry needling in painful, tight or restricted muscle groups. You may have heard about Trigger Points - those painful, tight bands that can form within a muscle over time, with repeated use or from injury. Dry needling is a technique that helps address these trigger point areas in a very specific and precise way. We assess the areas through watching you move and through palpating the muscles to find the best spots within the muscle to position the needle to relieve the trigger point. We also assess the surrounding joints and muscles, for example for hip pain we may find that dry needling in your lower back or in your thigh can help relieve pain and strain from your hip. What Happens When We Needle A Trigger Point? When we first insert the needle to the muscle, it can be felt as a little pinprick sensation on the skin. We then guide the tip of the needle into the right angle and depth of the muscle to directly stimulate the trigger point. This takes some skill and the ability to visualise in 3D the target muscle and the surrounding tissue like nerves, veins, arteries, bones and ligaments. By applying the needle into that trigger point, it causes a combination of chemical and electrical responses by the muscle. The micro damage causes by inserting the needle sends chemical messengers to the brain to get a healing response to occur. It can also cause a nerve impulse to occur, making the muscle twitch and release. To Stimulate or Not To Stimulate Because our aim in using dry needling is to get a change in the muscle tension, we often can stimulate the needle. This means we might gently move the needle in a pulsing in/out movement to repeatedly stimulate the trigger point, or we might twist the needle in a particular direction or in a series of back and forward movements. Stimulation of the needle can lead to more twitching, what we call Local Twitch Response. Dry needling can be effective even without the involuntary muscle twitch response. Some practitioners prefer a more intensive stimulation of the needles, however we prefer a gentle and slow approach. Does Dry Needling Hurt? In most cases, not really. Which is often surprising! The most common sensations you'll feel are the pinprick of the needle being positioned, a dull aching or tightening sensation around the needle, and the quick twitching response of the muscles releasing. The twitching can sometimes feel intense, but only lasts a very short time. After needling, some people can experience a little localised soreness at the sites of the needles, but most people just feel relief from tension and pain in those areas. Is Dry Needling Safe? In the hands of a trained practitioner, dry needling is a safe and effective technique. Myotherapists undergo many months of training and assessment in the skillful use of dry needling, however not all practitioners who offer dry needling are Myotherapists. Remedial Massage Therapists, Chiropractors, Physiotherapists, and other skilled practitioners can opt to undertake short courses in dry needling. Here in the Simple Wellness Myotherapy clinic, we only allow our Myotherapists to use dry needling on our patients, and we strongly believe that a weekend short course is not enough time to develop the skills needed to use dry needling safely and effectively. What Sort Of Pain Can Dry Needling Help Treat? Dry needling is great for releasing tight trigger point areas all throughout the body. It can be effective in treating headaches, neck and shoulder pain, back pain, bursitis, pain from disc injuries, sports injuries, plantar fasciitis - so many things! Want to try dry needling for your muscle pain? Book an appointment with one of our Myotherapists. Many people are familiar with the term "bulging disc" in regards to lower back pain. It can feel like an intense, sharp, stabbing sensation that can often travel down your leg through your hips and bum, sometimes as far as your feet. This is a common diagnosis when you start to develop back pain. You get a scan which shows changes in the disc, and the pain matches the effected nerve area. It can be a scary diagnosis. But you may be surprised to know that a lot of people who don't have pain have also been found to have changes in their discs. I find this study to be really encouraging, because it shows that people who have significant changes to their disc structure can still live a painfree life. It suggests that the disc changes may have already been there for some time before any painful symptoms even began, and gives hope that even if the structure doesn't change, that the pain can change. Lets have a look at this interesting literature review, particularly in regards to the findings around disc degeneration, disc bulges and disc protrusions. This is a literature review of 33 separate studies that investigated the imaging of spinal degeneration in painfree people ranging from their 20's to their 80's. It was published in the American Journal of Neuroradiology in 2014. In total, the review takes into account MRI and CT scan imaging on 3110 individuals with no painful symptoms. As you would likely predict, the number of findings increased with the participants age group, showing age-related degeneration occurs even in people who aren't experiencing pain. Lets have a look at the imaging results for the disc degeneration, bulge and protrusion categories: Disc degeneration - changes to the disc and surrounding vertebrae that result in loss of cushioning and support, may include signs of osteoarthritis at the joint. The Results: Disc degeneration in painfree participants was identified in:
Disc bulge - changes that alter the shape of the disc and can make portions of it "bulge" out of place, which can apply pressure to nearby nerves. The Results: Disc bulge in painfree participants was identified in:
Disc protrusion - changes to the annular membranes around the disc allows the disc nucleus to protrude and apply pressure to the nerves. The Results: Disc protrusion in painfree participants was identified in:
What does this mean for your bulging disc? It means that theres a good chance that your structural changes were already present before your back became painful. The area may be irritated or flared up right now, but these findings are a good indication that even if your scans don't change, your back pain still can settle down. It means that a scan showing disc changes doesn't have to be a life sentence of pain. Does this mean bulging discs DON'T cause pain, then? Don't get me wrong, bulging discs can be painful, and for some people it can be severe. This study just helps to show us that theres more to back pain that what shows up on MRI or CT scans. Structural changes are just one layer in the complex onion that is back pain. We can help! There are lots of ways we can change your experience of back pain through massage and myotherapy techniques like dry needling, taping and support, strengthening the surrounding muscles with exercises that are appropriate for you, and supporting your understanding of how your back functions. Book a time to come see us to talk about your back pain and creating a treatment plan to reduce it. If you have joint pain, chances are that hydrotherapy is going to be a huge help to you. A hydrotherapy pool is a warm water pool for doing exercises. Its quite different from swimming laps, although a lot of people find that swimming can be helpful too, if its not painful to do it. Can’t swim? It doesn’t matter, a hydrotherapy pool is usually quite shallow, it usually doesn’t have a “deep end” where you can’t touch the bottom. Our local hydrotherapy pool is at Knox Leisureworks in Boronia. The centre has a lot to offer, actually. There is the hydrotherapy pool, as well as a kids pool, a regular lap pool, a spa and sauna, and an onsite gym. So why is Hydrotherapy such a great option?
Buoyancy – Being in the water takes the pressure off the joint due to the water supporting your body weight. This makes it a great option for weight bearing joints like hips, knees and ankles, especially following injuries or surgeries like hip and knee replacements or fractured bones. Warmth – Heated hydrotherapy pools allow muscles to stay warm and relaxed while exercising. Typically a hydrotherapy pool is heated to about 33*, warmer than a normal swimming pool. Low Impact – Unlike running, doing exercises in water is friendly on vulnerable joints. The water doesn’t allow you to move as fast as in air, so the force of impact is less than running or jogging on a hard surface. Resistance – The water provides great resistance for strengthening the body, without feeling painful. It can be tiring afterwards due to the resistance of the water, though, so starting with short sessions is best. Low Cost – Knox Leisureworks has a great hydrotherapy pool. You can access the hydro pool with your standard pool entry fee of around $8, or if you plan to go frequently they have multi visit passes or memberships. What kinds of pains or conditions does it work well for? Hydrotherapy is fantastic for helping with pain in big joints and weight bearing joints, like hips, knees and ankles. Lower back pain can respond very well to hydrotherapy because of the way the water helps take pressure off the spine and support the weight of the body while you move. It can also be great for things like arthritis, and rehabilitation after a fracture or surgical repair. It can be great for general fitness, too! How do you get started? Initially just walking through the water can be really helpful. You can also include day to day movements like bending and straightening your knee or hip while standing with you back against the pool wall for support. You can use a floating board or pool noodle to hold onto and do gentle squats or lunges. If you’re uncertain, talk to us about specific pool exercises at your next appointment and we can help create a program tailored for you. |
Meet Our Team
We have a team of great practitioners available 7 days a week at our Rowville clinic. Archives
July 2024
Categories
All
|
Got a question about Myotherapy?
Contact Mel by phone, email or Facebook
|
Simple Wellness Myotherapy & Remedial Massage Clinic
Shop 12B 150 Kelletts Rd Rowville VIC 3178 |
Phone us on
03 8204 0970 |









 RSS Feed
RSS Feed