|
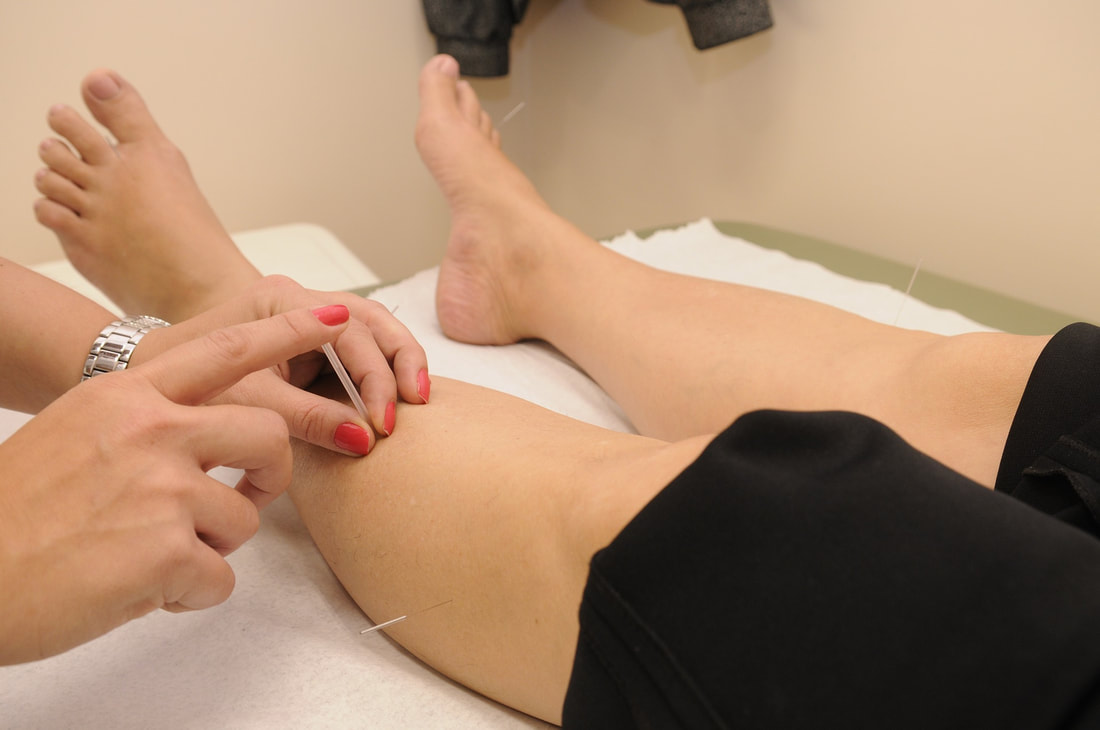
Most people have some idea about acupuncture, even if they don't know exactly how it works. But many aren’t sure about the difference between acupuncture needling and dry needling. This is a question that comes up all the time during myotherapy sessions! So let’s look at the key similarities and differences. The Similarities
First, let’s look at the common ground between the two forms of treatment. The needles Both use needles as the tool of treatment. These needles can come in various lengths and thicknesses depending on what they are used for. Needles should always be sterilised and single-use. The training Qualified practitioners have to be trained extensively in how to correctly needle a client. Learning where, when and how to use a needle on a human body is a bit intimidating, but it is essential for safety reasons. Whether you get acupuncture from a Traditional Chinese Medicine practitioner or dry needling from your Myotherapist, you can rest easy knowing there has been months or even years spent on training. However, dry needling courses can also be offered as short weekend courses for practitioners like remedial massage therapists, physiotherapists, chiropractors, etc. If I'm honest, I don't think these courses are long enough, in depth enough, and with enough assessment and examination of each participant. Acupuncturists and Myotherapists train for a long period of time, need to pass both written and practical exams, and complete student clinic treatments under supervision to build their needling competency. The Differences Now we get to the differences between the two forms of treatment. Why it’s done & what it treats Acupuncture is a Traditional Chinese Medicine practice, with thousands of years of use. It is used as one treatment form to bring the body back into balance according to TCM treatment protocols, the most familiar of these being the system of meridians, or energy points throughout the body. Acupuncture can be used to balance hormones, optimise digestion, reduce stress and treat a lot of conditions, including musculoskeletal issues. I'm always very honest with people when I say that I don’t understand the theory or application well because I’m not a trained acupuncturist, and I refer any more specific acupuncture questions to Amanda Cox-Edwards at Upwey Acupuncture. Dry needling is a modern physical therapy. It is used to correct imbalances in musculoskeletal health. The goal is to release tension in a muscle, returning it to its natural, neutral tone. Dry needling is used specifically for muscle and joint complaints, as a comparison to acupuncture which has more system wide applications. Where it is used Acupuncture can be used directly over an area of concern. But it can also be used distally – that is, a distant point on the body that is related to the area of concern according to the meridians. Certain points on the bodies surface relate to other areas, including internally. Of course, your acupuncturist won't needle directly into your kidneys to treat a kidney issue or into your intestines to treat a digestive issue, they will use the TCM protocols to stimulate points throughout the muscles and skin of your body that relate to the kidneys or digestive system. On the other hand, dry needling is used directly on the affected muscles. We find the muscle that is tight, spasming or needs to be released, and then locate the spots of most tension within that muscle and that becomes our needling target zone. How the needle is used The final major difference is how the needle itself is used as a tool. In acupuncture, the practitioner will insert the needle in the specific spot and depth and generally leave it to do its job while the client relaxes. This can be for up to 45 minutes, depending on what they are treating. Dry needling is not left alone. Instead, the practitioner will often try to stimulate the muscle fibres by moving the needle, helping to release the tension. The most commonly used stimulation techniques include an up-down motion to repeatedly hit the target within the muscle; a twisting action to wind and release the tissue; and in-out motions on an angle to release broader areas of tension. Some therapists take an aggressive approach to dry needling, and it can be uncomfortable or even painful to receive needling from this type of therapist. By now, you probably know that I'm your gentle Myotherapist, so in typical gentle fashion I use very slow, deliberate stimulation techniques where needed. I also like to let my needles rest then re-stimulate it a few minutes later, rather than continuous stimulation. Dry needling is just one tool out of a big, broad toolbox that Myotherapists have to use. Scared of needles? We have plenty of other ways to gently encourage your muscles to relax and release without needing to use needles on you. Does dry needling sound like something you want to try? The good news is that myotherapists have extensive and ongoing training in dry needling. So book yourself in a session to try it today. Remedial massage and myotherapy treatments are fantastic for releasing muscle tension and loosening up the tight spots. But unless you’re in the clinic a few times a week, there’s a good chance you’re still dealing with tight muscles in your daily life. There are heaps of contributing factors to tight muscles. How you move, how you sleep and how you spend your time can all affect your muscles. But one thing that you might not immediately think of is your diet. There are specific nutrients that your muscles need to contract (tighten) during movement and then relax during stretching or when you’re at rest. One well-known mineral is magnesium – also known as the relaxation mineral. So I asked my nutritionist bestie Sam Gemmell, aka The Rebel Nutritionist, for her top tips around using magnesium to keep your muscles in peak condition. My favourite fun fact from Sam is that dark chocolate is a great source of magnesium, and officially Nutritionist Approved! (Of course, in moderation!) Why do we need more magnesium?
Simply put, because we aren’t getting enough. Most people don’t consume enough through the diet. Magnesium is generally found in wholefoods, which we’re eating less of thanks to the increase in processed foods. But even for those who do eat enough, other factors such as chronic stress can deplete magnesium levels. If you have any kind of gut symptoms such as bloating, constipation or diarrhoea, you might not be able to absorb a good amount of magnesium from the foods you eat. There is also the issue of food containing less magnesium than previous years because the soils are being depleted of this vital nutrient. Magnesium is often called the relaxation mineral, but that’s too simple a term. It is used in over 300 different processes in the body. Healthy magnesium levels support energy production, muscle relaxation, blood sugar regulation, optimal blood pressure, bone strength and production of brain chemicals – just to name a few functions! Magnesium-rich foods to include The most sustainable way to boost your magnesium levels is to eat it! But the good news is that there are plenty of foods that contain magnesium. Some of the best options include:
As you can see, there is a variety of different options that cater to almost any dietary requirements. For best results, I’d recommend including at least one serve of magnesium-rich foods with every meal. This might mean: Oats, quinoa flakes or nut butter on wholemeal toast for breakfast Bean salad, fish and quinoa or sushi with wholegrain rice for lunch Adding a serve of green leafy vegetables to dinner (eg in your bolognaise sauce or soup) Other methods of boosting magnesium Sometimes, boosting your magnesium-rich foods is all you need to get results. But if you have very low magnesium levels, or have any kind of stress or condition depleting your levels, you might need to use food combined with other strategies. Supplements An easy way to get more magnesium in is with a supplement. That being said, please don’t just pick up a magnesium bottle from the supermarket! Magnesium supplements can vary from high-quality to very poor quality (which will give you nothing but diarrhoea!) The forms of magnesium found in most over-the-counter products can be irritating to the gut lining. These are best avoided for anyone with impaired digestion, absorption or any current gut symptoms. Your best bet is to see a practitioner who can recommend a high-quality practitioner brand. This also means you have some guidance around which supplement best suits your needs, as well as how much to take. You could even book a consultation with Sam at The Rebel Nutritionist, she would love to help you! Transdermal magnesium If you have issues with taking magnesium supplements or have very low levels, transdermal magnesium might be an alternative to try. The magnesium is absorbed through the skin. The exact amount of magnesium that makes it into your system isn’t well-researched, but some is better than none! You can use transdermal magnesium by using:
Muscles feeling tight? Been a while since your last myotherapy session? Click here to book a session. You might be familiar with that sharp, shooting pain sensation in your lower back, hip and leg. It can also be felt as numbness, pins and needles, tingling or burning type of sensations. Whatever way the pain or symptoms present, it runs along the Sciatic nerve - which is why this is referred to as Sciatica.
But did you know theres more than one potential cause behind this pain? Often this pain can be linked to muscle tension in the glutes and hips. The Sciatic nerve runs underneath the muscles of your glutes, and when it gets compressed there it can be a real pain in the bum - literally! Because this nerve runs all the way down to your feet, the jolts of nerve pain can sometimes be felt anywhere from just localised in your buttocks and hip, to the back of your thigh, behind the knee, straight down your lower leg and even into the base of your foot. The Sciatic nerve can be impacted at the root of the nerve near the spine, however this doesn't always mean there will be pain. Often this is called a Bulging Disc or Herniated Disc, but you might be surprised to learn that even though "Bulging Disc" sounds pretty awful, studies have shown that more than 50% of people over 40 with no pain symptoms at all can have a disc bulge show on scans. Irritation or compression of the Sciatic nerve can be common after serious trauma to your leg or lower back. Things like car accidents, falls, and horse riding accidents are all common high impact incidents that can aggravate the nerve. If you've had an injury like this, its wise to seek treatment for it. Do you have Sciatic nerve pain or nerve symptoms of numbness, tingling and pins and needles? Book an appointment with us to have an assessment and treatment. If we can resolve the issue, we'll create you a treatment plan that includes manual therapies and a take home exercise program. More serious causes do exist, so if treatment of the muscles and joints is not relieving your pain, we'll refer you to see your GP to rule out any serious structural or pathological conditions. We all know that our bodies are full of these things called nerves, but have you ever wondered how they work to control your body?
Lets have a look at two important types of nerves in your body - the ones that tell you sensory information like touch or taste, and the ones that move your muscles and joints. Sensory nerves are responsible for everything you feel or sense. The five senses - sight, sound, touch, taste and smell - all fall under this category. Any awareness you have of the feeling or sensation of your body comes from the sensory nerves. The main sub types of these nerve receptors are mechanoreceptors, chemoreceptors and thermoreceptors. Mechanoreceptors respond to pressure and touch. When you feel muscles stretch out, or when you're aware of the chair you're sitting on, thats all thanks to mechanoreceptors. Chemoreceptors send information about chemical changes. This could be like the warming feeling of rubbing Deep Heat over your sore shoulder, as well as internal biochemical changes, like lactic acid build up after doing a big workout. Thermoreceptors tell us about temperature. They respond when you touch something hot or cold, and are the reason you'll quickly pull your hand away from a hot stove to avoid a serious burn. Then we have your Motor nerves, these are the ones that control movement. Every time you make a movement, its because these Motor nerves are sending a signal from your brain to the muscle they activate saying "Move!" Fun fact - muscles can only ever pull, they can't push! So when you activate your biceps to bend your elbow the biceps muscle contracts and gets shorter which pulls your forearm upwards. When you want to stretch your elbow back out straight, your Motor nerves activate your triceps which then pull your forearm back down to straighten the elbow. Everything in the body is controlled by nerve signals. The brain is like the control centre, and the nerves move out from the brain into all the tissue of your body - muscles, joints, organs, the lot. Some nerves can be over a metre long, like the ones that send signals to and from your toes. The nerves in your arms and hands all connect in via your neck, which is why we like to assess and treat your neck if you're having any pain, or tingling or other "nerve-y" symptoms in your hands and arms. The same goes from the nerves for your feet and legs - they extend out through your lower back, which is why we consider your back when you come in for treatment for your foot, ankle or leg. How can you tell if your pain or symptoms are nerve related? If a Sensory nerve is involved in your pain it can feel like sharp, shooting pains, tingling, pins and needles, numbness, or just feeling "weird" (we call that parasthesia) If its a Motor nerve thats involved, the muscle groups that nerve activates can be weak, or in extreme situations might not be able to activate at all. If you think your symptoms may be nerve related, book in with your Myotherapist for a full assessment and treatment plan. We know that it’s good to move our bodies on a daily basis. But when we get injured, it’s a good excuse to chuck in the towel for a few weeks– right? Wrong! Exercise or at least some type of movement is an important part of your recovery process. Although it might not be good to go for a run 2 hours after you break your ankle (ouch!), you do want to incorporate movement as your body heals. Let’s look at why exercise is so beneficial, and how to include it safely. What are some of the general benefits of exercise?
So first up – why do we want to exercise on a regular basis? I’m glad you asked! There are so many benefits to exercise for your physical, mental and emotional wellbeing. Some of them include:
Exercise, injury and pain The old-school approach to pain was all about rest and inactivity. But now we know that movement done correctly is one of the best things you can do for pain. When it comes to pain and injury, research has shown that exercise can:
But there are also the indirect benefits. For example, exercise improves sleep, which is when your body does its best healing. If you’re not sleeping well, it will take you longer to heal. But if you use exercise to improve your sleep, it can boost your recovery. How to exercise safely after an injury Convinced that you need to move that body? Let’s go about this with safety in mind. Here are a few tips to get you started. Start slow. After an injury, there are a lot of complex processes going on. So the last thing your body needs is for you to try and run a marathon while it’s still healing! Begin with gentle movements, and work your way up over a period of weeks until you’re back to your pre-injury levels. Use your non-painful joints. If you have an injured upper body, use your lower body for exercising. If you’ve got an injured lower body, do some upper body exercises. Endorphins don’t stay in the one place – they are systemic. So if you’re moving non-sore parts, the endorphins will make their way around your body to the sore parts to help relieve the pain. Get a proper rehab program prescribed. This might not be necessary if you’ve only rolled your ankle or stubbed your toe. But if you have had a significant injury or are in significant pain, it’s best to get help. As a myotherapist, I can prescribe rehab exercises that build your body’s strength back up, and adapt exercises that might be causing pain. Your exercises will change throughout our treatment plan - we start from light, easy exercises while the pain or injury is acute, and work up to more challenging exercises to rebuild strength when your body is ready for it. Ready to book in a session? Head to the booking page here. As a myotherapist, I see my fair share of weird and wonderful injuries. But one of the most common injuries that requires proper rehabilitation is a dislocated joint. So let’s look at all the things you need to know if you’ve dislocated a joint. What is a dislocation?
A dislocation is the full displacement of a bone at the joint. So the bone is moved to somewhere outside of the joint it belongs to. Dislocating a joint is incredibly painful for most people. But along with short-term severe pain, it can also predispose someone to chronic pain if not rehabilitated correctly. Why do dislocations happen? Generally, dislocations occur due to high-impact trauma to the joint – think car accidents, falls, fights or high-impact sports like football and rugby. However, if you have a joint that is weakened or unstable, it could be caused by something with minimal force. This is commonly seen in people with hypermobile joints or a hypermobility condition. Joint shape differences such as hip dysplasia or variations in the shape of shoulder bones can also increase risk of dislocation. Joints that are at risk of dislocating Pretty much any joint in the body can be dislocated if there’s enough force. But some have a greater risk of dislocation because of their location and/or their structure. They include:
Dislocation red flags to watch for If you’ve experienced a dislocation, there are a few things to keep an eye on. These can often warrant medical attention.
The rehab process for dislocations This can depend on the type of dislocation. The greater the damage to muscles, tendons or ligaments, the longer the process of rehabilitation. For some people, recovery will take a few weeks, and they will regain their full strength. For others, they are starting with almost no function or stability. So for those people, it’s like learning how to use the joint from scratch. A history of previous dislocation to the same joint can also mean a longer rehab, as you’ll be attempting to heal twice the damage (or more!) to regain full function. What can a myotherapist do for dislocations? So you’ve dislocated a joint, and you want to know what your friendly local myotherapist can do for you. Here’s what I can do to help you recover!
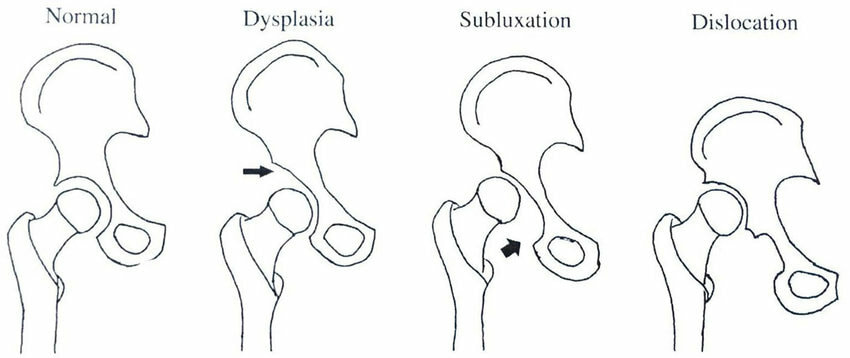
What I CANNOT do is help you relocate a joint that is still dislocated. Relocating dislocations is a medical procedure that is out of my scope as a practitioner. If you come to the clinic with a dislocated joint, I’ll send you straight over to the Angliss for medical attention! So do yourself a favour and skip the myotherapy session until your joint has been relocated by a medical professional. Are you recovering from a dislocation injury? Head on over to my booking page, so we can start strengthening your injured joint and get you back to living life! Most people understand joint dislocations. But subluxations, or partial dislocations, are a bit different. As a myotherapist, I see plenty of subluxations and related injuries every week. So let’s look at why subluxations aren’t quite dislocations, and what you can do about them! What is a subluxation? Unlike a dislocation, a subluxation is a partial displacement of the joint. With a dislocation, the bone is completely out of the joint it belongs to. But with a subluxation, the bone is only partly out. Just because it is not a full dislocation doesn’t mean that it won’t hurt! Subluxation can still be painful, as the joint is being wrenched out of its usual spot. It can also leave you at higher risk of chronic pain if the joint isn’t rehabilitated after the injury. In the image above, we're looking at the ball and socket joint of the hip. The Normal hip joint shows the ball of the femur (thigh bone) sitting neatly inside the socket joint of the pelvis. In Dysplasia, the shape of the socket is not correctly formed so the socket doesn't snugly hold the ball of the femur. In Subluxation, the ball of the femur has partially slid out from the socket, and while its still almost in the right spot, it likely won't move smooth and painfree like the normal hip. And in the Dislocation, the ball of the femur has entirely moved out of the socket.
Why do joints sublux? It is easier for a joint to sublux than it is to dislocate. That being said, if you have full strength and integrity in your joints, it will take a high-impact injury to sublux a joint. This is usually something like a fall, car accident or a sports injury. However, some people are at a higher risk due to weak, unstable or unusually shaped joints. A previous history of dislocation or subluxation can weaken the joint and make it more prone to a sublux. People with hypermobile joints can sublux joints with minimal force, because the ligaments (connective tissue that holds the joint together) are more elastic than they should be. This can lead to the person being very flexible but also more prone to subluxations – some of my more hypermobile clients can sublux joints while walking, sitting, or even sleeping! You can also have variations in the shape of your hip or shoulder joints that make it easier to sublux. Hip dysplasia is one common variation that increases the risk of subluxing a hip joint, like in the image above. Joints at risk of subluxation In the clinic, I’ve seen almost every subluxation possible, thanks to my hypermobile clients! But there are several joints that are easier to sublux due to their location and structure:
If you have hypermobile joints, you may be at risk of subluxing other joints like ribs, jaw and collarbone. How is a subluxed joint rehabilitated? It can depend on the type of subluxation, and how it occurred. If it was due to high-impact trauma, there’s likely to be a decent amount of joint damage that needs attention. It could take weeks before the pain subsides enough to focus on rehabilitation. But if the sublux occurred due to hypermobility or dysplasia, it might just need a little TLC for a week or two. After that, the focus will be on building up the muscles that support the joint to reduce the risk of recurrence. Either way, the focus for rehabilitating the joint will include stabilising it, minimising any symptoms, and rebuilding the strength and integrity. What can a myotherapist do for subluxations? If you’re dealing with a subluxed joint (or multiple!), I’m here to help. Let’s look at how myotherapy can help with subluxations:
So don’t sit at home and feel sore after a joint has subluxed. Come see your favourite myotherapist. We’ll have you feeling better in no time! Click here to book an appointment. A lot of people who don't have persistent pain don’t realise how much chronic pain sucks. Ongoing pain isn’t just about physical discomfort – it also affects your mental wellbeing, your social life and your long-term health. This is why I have such a strong focus on chronic pain management as a myotherapist.
But what can myotherapy do to help with chronic pain? I’m glad you asked! One of the things I love about myo is that it has so many tools, so there is always one that can suit your needs and tolerance. Here are the main ways I use myotherapy techniques to help you manage chronic pain. It helps to manage acute flare-ups When you have chronic pain, it’s common to have a flare-up of symptoms and/or pain levels. Sometimes it can be your nervous system increasing your sensitivity, and sometimes it’s a physical factor such as tight muscles that cause issues. Either way, different techniques such as taping, massage and mobilisation can relieve the flare. It can down-regulate the pain response One of the main problems with chronic pain is that the body becomes more sensitive to pain messages sent by the nervous system. Sometimes the number of connections along nerves can be altered. Other times, there is a greater release of neurotransmitters, which makes the body super-sensitive to sensation. I cover this a bit more in my pain matrix article, but non-painful sensations can block the danger messages. This means that pressure from a gentle massage or myofascial release stretching can help to reduce pain. It can look at the root causes behind chronic pain There are so many factors that can lead to chronic pain, and even more that can aggravate it. But as a myotherapist that focuses on chronic pain, it’s my job to be an investigator into your pain. Your treatment plan might include exercises and stretches that aim to correct any underlying causes of pain. We’ll also have regular discussions about the lifestyle factors that might be contributing, and ways to modify them. And if I think one of your triggers is out of my zone, I’ll refer you to a trusted practitioner who also works with chronic pain. It can reduce stress hormones Want to hear something cool? The relaxation after a myotherapy session isn’t all in your head. Research has found that massage can reduce cortisol, your main stress hormone, by 31%. As a bonus, it can also boost your levels of feel-good brain chemicals serotonin and dopamine. If that isn’t a good reason for regular myotherapy sessions, I don’t know what is! It can release trigger points Ever had a little knot feeling on a muscle, that when pressed, feels so sore but so good? That’s a trigger point. These taut bands are like a micro-spasm of a muscle (not a full muscle spasm like if your leg cramps in the night!) Trigger points can contribute to chronic pain, and they can certainly exacerbate it. Because trigger points tend to have referral patterns, they can also make you feel pain outside of the area that the actual trigger point is found. As part of your myotherapy treatment, I can release any problematic trigger points around the area of pain. For example, if you have chronic headaches, I might look at the trigger points around your head, jaw and shoulders. Tape can be used to stabilise joints if needed If your chronic pain comes with any joint instability, taping is a great tool for managing it after you leave the session. By using either rigid or kinesiotape, depending on the issue, we can stabilise the problem joint or joints. That way, your painful area is supported and you’re less likely to make movements that aggravate the pain. The tape can also be used to help continuously guide and remind your joints of a better position to rest in which helps to take strain off certain areas. Looking to manage your own chronic pain? Your no-pain, all-gain myotherapist is here to help. Head here to book your appointment today Everyone has experienced pain at one time or another. But pain is personal – each of us experiences pain differently. Some of us feel it very intensely, and others not so much. This is because pain depends not only on what happens to your body, but also how your brain responds to it. This is what is known as the Pain Matrix. What is the Pain Matrix?
This matrix processes information from the nerves that tell us when we’re in danger or injured. It responds by increasing or decreasing our sensitivity to these messages. These changes – known as top-down regulation – control how intensely we feel pain. The Pain Matrix involves different areas of the brain that control emotions, behaviour, movement, perception and thoughts. So it’s no surprise that when you’re in pain, all of these different factors can change. How does the Pain Matrix work? There are two main changes that the Pain Matrix can induce. Anti-nociception is a reduction in sensitivity to pain, whereas pro-nociception is an increase. Anti-nociception uses the body’s natural painkillers – endorphins – to block the danger signal and decrease the pain response. Ever seen someone injure themselves in a dangerous situation, like in a car accident, but they can still move to safety without feeling pain? This is because a rush of endorphins temporarily blocks out the message of danger so they can get to safety. On the other hand, pro-nociception is usually due to swelling and chemical changes in the nerve endings around an injury. Have you ever had a bad paper-cut? Your sensitivity is much higher around the cut, even if you’re not touching the injured part. Sometimes, even moving the other fingers can hurt. Changes in the brain = changes in the pain Despite what we used to believe, the brain can continually change its form and function as a form of adaptation. These changes are known as Neuroplasticity. Nerve pathways can physical alter by increasing or reducing the number of connections. Or they can alter the release of neurotransmitters – more stimulating neurotransmitters means more nerve activity, which can increase the sensitivity of the system. When it comes to chronic pain conditions, the central nervous system is reorganised. This can include damage to nerves, leading to abnormal connections between them. Pain is more likely to occur than not, as pro-nociception increases and anti-nociception is impaired. This can lead to exaggerated responses to pain including pain caused by non-painful experiences - this is known as allodynia, and can be a common symptom in conditions like Fibromyalgia. Long term inflammation can lead to a heightened sensitivity of the nervous system. In the presence of inflammation the amount of nerve stimulation needed to send the signal decreases and the nerve firing rate increases. With so many danger messages coming in when there is inflammation present, the nervous system starts to respond on high alert by using its protective mechanism - pain! Controlling the pain There is no one size fits all approach to controlling pain, but theres increasing evidence that changes to pain intensity can be influenced by more than just the incoming messages from our tissue - it can also be influenced by our perceptions of danger and safety. This is likely due to the pain matrixes involvement in areas of the brain that deal with emotions, behaviours and thoughts. Pain experts Dr Lorimer Moseley and Dr David Butler of the NOI Group have published a fantastic book called Explain Pain that describes DIMs and SIMs - that is, Danger In Me (DIMs) and Safety In Me (SIMs). They say that any credible indication of danger can increase your perception of pain, and likewise a credible indication of safety can decrease the pain. We'll dive deeper into this research in future blogs. The Gate Control Theory involves a more physical approach to pain control. Have you ever bumped into something, then rubbed the area to make it hurt less? The Gate Control Theory is that non-painful sensations such as pressure can block or override the danger messages and reduce pain. The nerves that tell us about pressure are faster and more effective than those that tell us about danger. This might be part of why something like a good massage session helps with pain. Massage is also a great way to stimulate some feel-good endorphins, which promotes anti-nociception to reduce painful sensations! If you’re looking to minimise your pain, a combination of massage, exercise therapy and other myotherapy treatments can help. Have a look at my online booking calendar to book in for an appointment. Headaches can vary from mildly dull and annoying to intensely sharp or throbbing. They can creep in slowly, or seem to appear out of nowhere. For some people they can last for a very short time, and others get headaches that just don't seem to quit. No matter what the cause of your headache, these simple tips are a great first step to help you to feel a little bit better. Suss out the origin
First up, you want to figure out why you have a headache. Have you spent too long at the computer without moving over the last few days? Have you been under a lot of stress? Have you lifted or carried something heavier than you're used to? Are you dehydrated? Or could it be hormone related? Having an idea of why you have a headache can help you figure out if you need help from your Myotherapist for muscle related pains, or if you need to make some changes to your routine like drinking more water or finding ways to reduce stress. Check in with your muscles Most headaches have some kind of muscular involvement, whether it’s directly causing the headache or is a side effect of the pain. The good news is that you can figure out if your muscles are involved. Have a feel along your neck and shoulders for any trigger points – spots that are tender and a bit painful to touch. Strong trigger points can send referred pain to other muscles, too. These are signs that your muscles are feeling tense, maybe from more physical activity than you're used to, or from staying in one position for a long time. Sometimes even your arms can have trigger points, so have a feel around your upper arm, particularly along the tricep area on the back of your arm. Have you been clenching your teeth? Feel around your face and jaw to check if there are any super-tender areas. You might also find a tight band around your temples. Headaches can be an early sign of TMJ dysfunction, so make sure you see your friendly myotherapist quick-smart if you are getting headaches caused by clenching or grinding. Are you getting sick? Another common cause of headache is sinus pain. Try gently pressing between your eyebrows and on either side of your nose, right below the eyes. If this area is tender, you might have a case of sinusitis coming on, and you'll probably have other symptoms like a runny or blocked nose and a fever. If you have a cold or infection, its always best for both of us if you wait til you've recovered from the contagious phase of the infection before you come in to see me. Check in with your pharmacist for a recommendation for something that can help with your cold/flu or infection symptoms - clearing the infection can often clear the headache! Something I can vouch for personally is Salt Therapy to speed up the time it takes for a sinus infection to clear. The salt helps with inflammation in the nose and lungs, as well as breaking up the congestion and making it easier to clear the sinuses which hugely relieves the pressure. Natalie at Salts of the Earth in Boronia takes care of me when I feel a sinus infection or cold coming on. Have a good stretch Remember those muscles from the last tip? They are the ones we want to stretch out gently. Roll your neck up and down, then side to side, breathing into any tight or sore spots. My little bonus tip here is to sit on your hand or hold the base of your chair so that you can really isolate the stretch into your neck and shoulders - when you're super tight, sometimes what should be a neck stretch becomes the whole upper body moving at once! Locking down your shoulder by sitting on your hand will help you feel a much more satisfying stretch into your neck! Open and close your jaw slowly, stretching out the muscles and releasing tension. Using your fingertips to massage over your jaw while you open and close can also feel really relieving! Reach your arms back behind your body for a stretch that targets the front of your shoulders, then roll down slowly as if you were trying to touch your toes for a nice back stretch - it doesn't really matter if you can or can't actually get to your toes, its more the stretching action here that counts. You can even bend at the knees if you feel too much strain in your hamstrings and the back of your legs. Drink some water! Most of us don’t drink enough water – myself included. But dehydration can cause headaches, and make them worse even when it’s not a direct cause. If you feel a headache rolling in, drink 1-2 cups of water. It can’t hurt, so why not give it a try? Is stress playing into your headaches? What does your down time routine look like? If its a bit neglected, try to find some time for things that you enjoy that can help reduce stress. For some people, that could be exercise or meditation - which are both fantastic for getting your brain to release some lovely happy hormones and neurotransmitters! But it might also be reading, gardening, seeing a friend, going out for a meal, playing a game. Remember – headaches and migraines are two different things! A super-bad headache does suck, but it feels different to a migraine. I’ll be sharing more on migraines in the future, but there are a few telltale signs. It’s probably not a migraine unless you experience at least a few of these:
If you have a headache that is being caused or worsened by tight muscles, I’m here to help. A Myotherapy treatment for headaches will look at your head, jaw, neck and shoulders, and could include some feel-good remedial massage to release tight muscles, as well as other approaches like cupping, needling or mobilisations to reduce pain and improve your movement. Book in a short session today, and we’ll have you feeling better shortly. |
Meet Our Team
We have a team of great practitioners available 7 days a week at our Rowville clinic. Archives
April 2024
Categories
All
|
Got a question about Myotherapy?
Contact Mel by phone, email or Facebook





 RSS Feed
RSS Feed